By imposing then lifting a ban on elective surgeries, Gov. Walz has created a ‘surge’ of non-Covid-19 ICU cases
Preparing for the peak
When, on April 8th, Gov. Walz extended his stay-at-home order (SHO) to May 4th, he did so because the SARS-CoV-2 (COVID-19) Model produced by the University of Minnesota School of Public Health and Department of Health told him that by doing so he would push the peak of Intensive Care Unit (ICU) usage of 3,700 beds back to July 13th. This would allow more time to build up the ‘surge capacity’ needed to cope.
The time appeared to have been used well. On April 29th, Gov. Walz announced:
I today can comfortably tell you that, when we hit our peak — and it’s still projected to be about a month away — if you need an ICU bed and you need a ventilator, you will get it in Minnesota.
Coming up short anyway
So it was alarming to read a story in the Star Tribune dated May 23rd titled ‘Minnesota health officials call for caution after news of Twin Cities ICU beds filling up‘. The report began:
Metro hospitals are running short on intensive care unit beds due to an increase in patients with COVID-19 and other medical issues, prompting health officials to call for more public adherence to social distancing to slow the spread of the infectious disease.
It is true that ICU hospitalizations have risen, as Figure 1 shows. On April 29th, there were 119 Minnesotans needing ICU treatment for Covid-19. At the time of the article that was up to 233. As of yesterday, it had reached a peak of 258.
Figure 1: Minnesotans hospitalized with Covid-19

Source: Minnesota Department of Health
But remember that a surge was forecast by Gov. Walz’ model back in early April. Indeed, as Fox 9 reported at the time:
Minnesota will need at least 3,000 intensive care beds when the infection peak hits in May through July, Malcolm and Walz said.
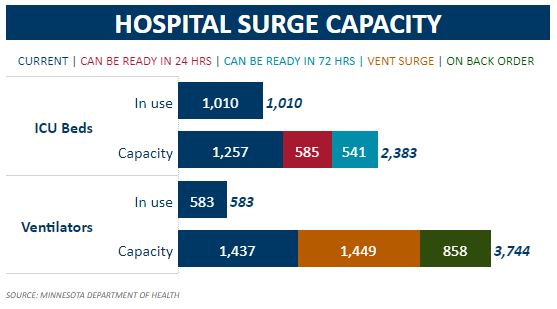
It is nearly June and we are nowhere near that. Indeed, the state government reports that there are currently 1,257 ICU beds in Minnesota (of which 1,010 are in use) with another 585 available at 24 hours notice and a further 541 available at 72 hours notice, as Figure 2 shows.
Figure 2:
Source: Minnesota Department of Health
Also remember that, a month ago, Gov. Walz told us “when we hit our peak…if you need an ICU bed and you need a ventilator, you will get it in Minnesota”.
The question has to be asked: why the reports that we suddenly find ourselves on the verge of being swamped?
The ‘surge’ is in elective surgeries
The Star Tribune report provides some clues. It reads:
…hospital officials reported that 95% of ICU beds in the Twin Cities were filled by patients with COVID-19 or other unrelated medical conditions.
Patients with unrelated medical problems needed intensive care, along with patients recovering from surgeries — including elective procedures that resumed May 11 after they had been suspended due to the pandemic.
“We are tight,” said Dr. John Hick, an emergency physician directing Minnesota’s Statewide Healthcare Coordination Center. “Resuming elective surgeries plus an uptick in ICU cases has constricted things pretty quickly.” [Emphasis added]
As the Star Tribune reported on March 20th, Gov. Walz issued an executive order telling hospitals to:
…postpone elective surgeries because of the COVID-19 pandemic emergency, a move that is designed to conserve resources as well as protect patients and caregivers.
On May 5th, as the Pioneer Press reported, he:
…signed an executive order…allowing health care providers to restart elective surgeries and procedures next week, if they have a plan for maintaining medical supplies needed for the fight against COVID-19.
ICU patients are either Covid-19 patients or non-Covid-19 patients. Gov. Walz’ model told us in early April that we would see a surge in Covid-19 ICU cases. That seems to be here but is much slower than forecast. But by imposing a ban on elective surgeries and then lifting that ban, Gov. Walz has created a simultaneous surge of non-Covid-19 ICU cases, as Commissioner Malcolm confirmed yesterday.
My colleague Tom Steward has already noted the ill-effects for patients of postponing these surgeries. It may well turn out to be a self-imposed handicap in Minnesota’s fight against Covid-19 too.
John Phelan is an economist at the Center of the American Experiment.