Minnesotans have eradicated the flu by masking and distancing. So how did Covid-19 survive?
Minnesota’s flu numbers are way down this year…so far
A month ago, I noted that the surge in Covid-19 hospitalizations in Minnesota – both ICU and non-ICU – had been largely offset by a fall in non Covid-19 hospitalizations. I wrote:
On the face of it, this seems strange. Why should non-Covid-19 hospitalizations be taking such a sharp fall? We are heading into flu season which typically sees hospital admissions rise, putting great pressure on hospital capacity even in years with Covid-19 to contend with. Why is this year so different? My guess is that many of these Covid-19 ICU hospitalizations are ones which would have occurred anyway given the usual seasonality, but are being logged as Covid-19 hospitalizations this year.
Support for this argument came quickly. A little over a week ago, I wrote:
Figure 3, from the Department of Health’s latest Weekly Influenza & Respiratory Illness Activity Report shows that, this year, we are seeing near record low hospitalizations with flu.
Figure 3
Source: Department of Health
This is something to watch closely in the next few weeks.
A week on, the numbers are shown in Figure 1. As bad as the Covid-19 situation might be in Minnesota this winter, we are, so far, having one of our best recent flu seasons. As Greta Kaul writes for Minn Post:
It’s still quite early in what’s typically flu season, but so far, numbers collected by health agencies offer encouraging news: they suggest transmission of the flu virus in Minnesota, as elsewhere, is minimal, especially compared to some years past.
Figure 1:
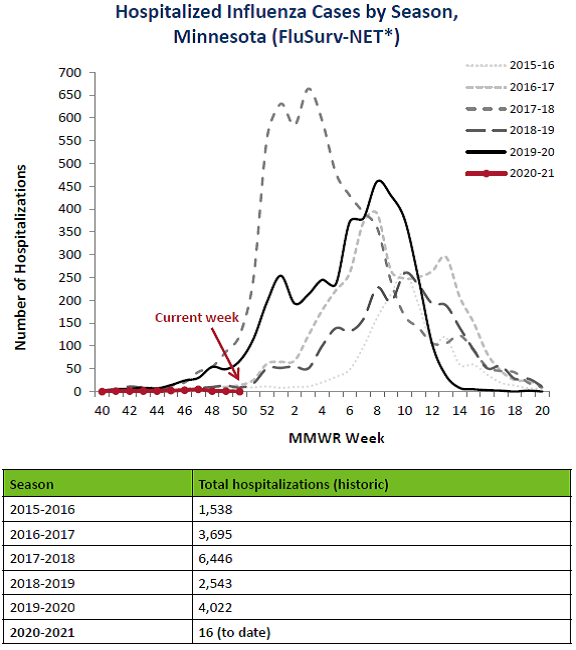
Source: Department of Health
Masks and social distancing killed the flu
Why might this be? Kaul suggests that:
It makes sense that there would be less flu transmission, given the precautions people around the globe are taking to slow the spread of COVID-19.
COVID-19 and the flu are both respiratory viruses that chiefly spread via respiratory droplets.
“[Droplets] happen when people cough, sneeze or even just talk, so those droplets are in the air and then they can get into peoples mouths or noses,” said Dr. James Smith, a third-year family U of M medicine resident at the U’s Broadway Clinic.
For both viruses, that’s especially likely to happen when people are within a 6-foot distance of one another for more than a fleeting moment. This is why social distancing — staying six or more feet away from people in social settings, and wearing masks that limit the amount respiratory droplets expelled, are effective for reducing both.
Indeed, that does make sense.
So why haven’t they killed Covid-19?
All of this is good news but it does beg a question: if we have been masking up and social distancing so effectively, how have we still had a large surge in Covid-19 cases?
Even with a mask mandate in place since July 25th, Minnesota saw a surge of Covid-19 cases, hospitalizations, and deaths starting in mid-September. When you pointed this out, the reply often came that the mask mandate wasn’t effective because people weren’t following it. In fact, data showed that Minnesotans were following the mandate. The numbers for flu – so far – support this. If we have been masking up and distancing to the extent that we have all but eradicated flu this season, then non-compliance with the mandate cannot be to blame for the surge in cases. We have either been complying or we haven’t.
‘Mask Karens’ have been stridently declaring on social media that our Covid-19 worries would be greatly reduced if we just obeyed the Governor’s orders more completely. The evidence doesn’t support that contention at all. The data shows that 95% of Minnesotans are wearing masks as required and the elimination of flu this year suggests that that is correct. The truth is that the effects of mask mandates are much less than many believe. This is not to say that they are pointless, but we should certainly stop shrieking at people about them in the comments.
John Phelan is an economist at the Center of the American Experiment.
