Minnesota’s COVID-19 emergency has passed. Why haven’t Gov. Walz’s emergency powers?
A version of this op ed appeared in the Duluth News Tribune, September 20th, 2020
When he closed Minnesota’s bars and restaurants on March 16, Gov. Walz said, “We’re not going to stop this from spreading, but we can stop how fast it spreads and we can make sure that we protect those most vulnerable.” When he issued a stay-at-home order on March 25, he said: “The objective of everything we’re doing here is, it’s too late to flatten the curve as we talked about, the testing regimen was not in place soon enough for us to be able to do that, or expand it enough. So what our objective is now is to move the infection rate out, slow it down, and buy time so that the resources of the ICU and the hospitals and the things that we’re going to talk about today can be stood up to address that.”
The point of the closures and the stay-at-home order was not to kill the coronavirus but to slow its spread so that the health system’s ability to cope would not be overwhelmed: “The thing that Minnesota is going to do is ensure if you need an ICU, it’s there,” Gov. Walz explained.
He was being guided by the University of Minnesota and Minnesota Department of Health’s SARS-CoV-2 (COVID-19) model. On April 10, Version 2 of this model forecast a peak of 3,700 Minnesotans needing ICU treatment for COVID-19 on July 13.
So, it was good news on April 29 when Gov. Walz announced: “I today can comfortably tell you that, when we hit our peak — and it’s still projected to be about a month away — if you need an ICU bed and you need a ventilator, you will get it in Minnesota.” When Version 3 was unveiled on May 13 and forecast a peak ICU usage of 3,397 on June 29, the state was equipped to handle it.
In the event, the peak — so far — was nowhere near as bad as the forecast, coming on May 30, with 263 Minnesotans needing ICU treatment. Following a string of such failed predictions, the model has now been quietly abandoned.
The disaster in our state’s care homes apart (we have had more COVID-19 deaths in our care homes than 25 states have had in total), the aim of the stay-at-home order of March 25 was achieved: Our health system has had more than adequate capacity to handle all COVID-19 cases needing ICU care. According to the Minnesota Department of Health, as of Sept. 17, the state has 1,046 ICU beds out of 1,222 in use with a capacity of 2,182 available at 72 hours’ notice.
This could change. There is still much we don’t know about this virus. According to the Department of Health, diagnosed cases surged from an average of 314 for the seven days up to and including June 16 to an average of 749 for the seven days up to and including Aug. 30.
But, over the whole 10 weeks of this surge in cases, we saw no such surge in hospitalizations. ICU hospitalizations, the health department said, surged from an average of 111 for the seven days up to and including July 18 to 154 for the seven days up to and including Aug. 10 — still below any time between May 6 and June 29. Since then, the numbers have trended downward again. In the seven days up to and including Sept. 17, the average number of ICU hospitalizations for COVID-19 in Minnesota was 135. The number of non-ICU hospitalizations has fallen from an average of 173 for the seven days up to and including Aug. 31 to 107 for the seven days up to and including Sept. 17.
Figure 1: Covid-19 non-ICU hospitalizations, ICU hospitalizations, and diagnosed cases in Minnesota
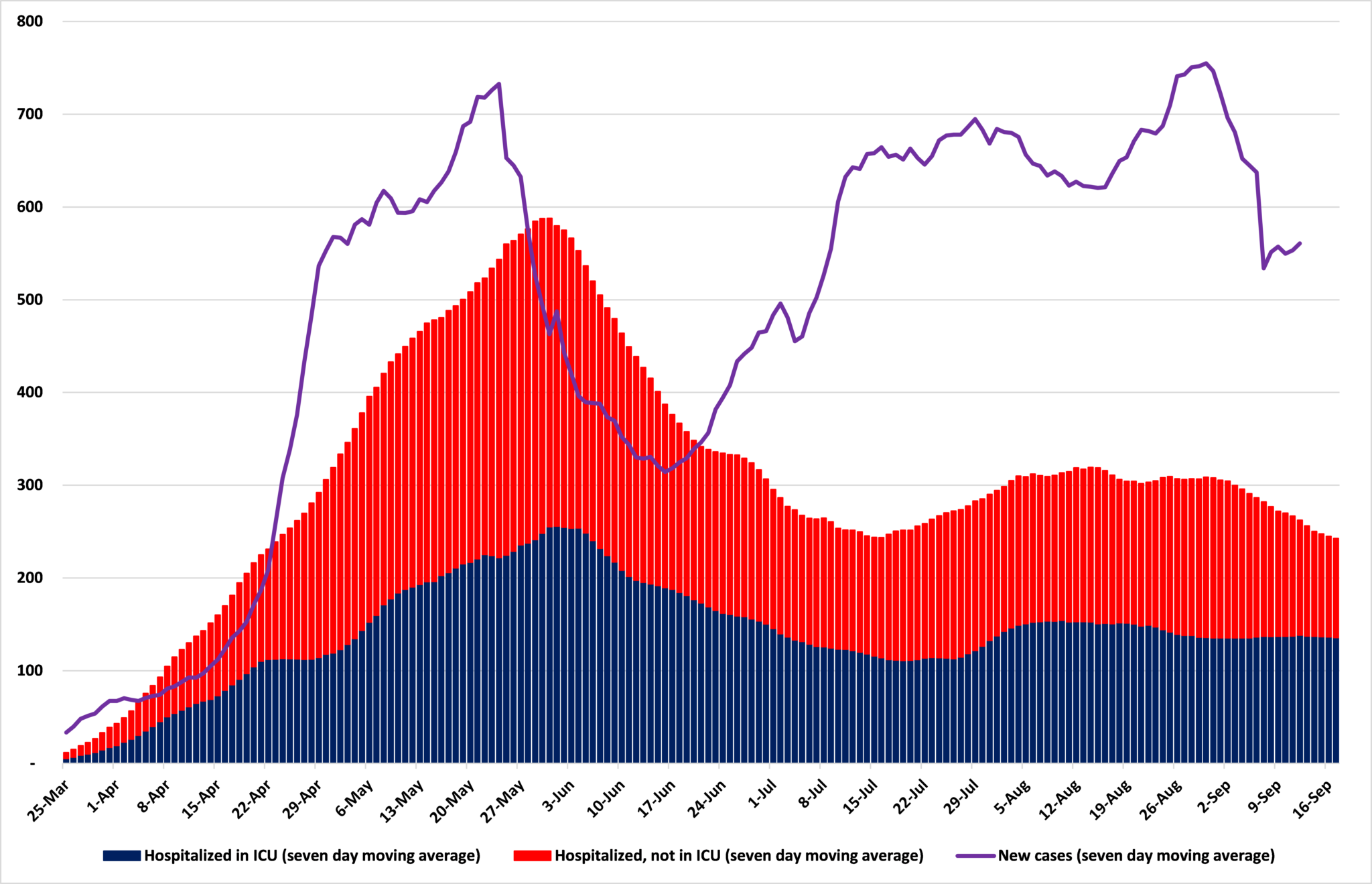
Source: Minnesota Department of Health
We are constantly being urged to look at the data. Here it is. While our fellow Minnesotans continue to die of COVID-19 and while each one of these deaths is a tragedy, the data clearly show that we have done what we set out to do back in March. Our health care system has not come close to being overwhelmed.
This month, Gov. Walz, rubber stamped by the House, extended his emergency powers for another month — but it is unclear why. While it is possible these numbers could surge, a possibility does not constitute an emergency. If it did, we would be in a permanent state of emergency.
For the time being at least, while COVID-19 is still with us, the data is clear: The emergency period of this pandemic is over.
John Phelan of St. Paul is an economist at the Center of the American Experiment (AmericanExperiment.org), a public-policy nonprofit based in Golden Valley, Minnesota. He wrote this for the News Tribune.